- Home
- About
- Portfolio
Crush the Match – Medical School and Residency Platform
Food¢ense – Curbing Childhood Obesity and Food Waste
HealthStack – Shared and Jailed HIPAA Hosting $50
Marta Care – Let Us Help When You Can’t
MD Idea Lab – We Build Prototypes for Doctors
Nervcell – The Healthcare Web Browser
Patient Keto – Personalized Keto Medicine and Telehealth
SwipeChart – Rapid EMR Interface
Treatment Scores – Quantifying the Science of Medicine
Treatments – Diagnosed. Now What?
VIDRIO – Google Glass and EMR Interface
- Blog
- Contact
Category: Health IT
Unlocking the Power of Health Informatics: Why It Matters
Introduction
Health informatics is a rapidly growing field that combines healthcare, information technology, and data science to transform the way we manage and utilize health-related information. In the digital age, health informatics plays a pivotal role in enhancing patient care, improving healthcare processes, and driving medical research. In this article, we delve into the importance of health informatics and the manifold ways in which it positively impacts the healthcare industry.
Enhanced Patient Care
Health informatics improves patient care by providing healthcare professionals with instant access to accurate and up-to-date patient information. Electronic Health Records (EHRs) store patient histories, test results, medications, and treatment plans, reducing the risk of medical errors and ensuring that the right treatment is delivered to the right patient.
Efficient Healthcare Processes
Health informatics streamlines administrative and clinical processes in healthcare. It reduces paperwork, automates scheduling and billing, and facilitates communication among healthcare providers. This efficiency not only saves time but also reduces costs, making healthcare more accessible.
Data-Driven Decision-Making
Health informatics leverages data analysis to inform healthcare decisions. By analyzing trends and patterns, healthcare providers can make more informed choices about patient care and resource allocation, ultimately improving patient outcomes.
Telemedicine and Remote Monitoring
The integration of health informatics in telemedicine enables remote consultations and monitoring of patients. This is particularly crucial in reaching patients in underserved or remote areas, providing access to quality healthcare that might otherwise be unattainable.
Public Health Surveillance
Health informatics supports public health initiatives by monitoring the spread of diseases and identifying potential outbreaks. Surveillance systems can help health agencies respond swiftly to emerging health threats.
Medical Research and Innovation
Health informatics aids medical research by facilitating access to vast pools of patient data. Researchers can analyze this data to discover new treatments, study disease trends, and develop innovative medical technologies.
Patient Engagement and Empowerment
Health informatics encourages patients to take an active role in their health. Patient portals allow individuals to access their own health records, communicate with healthcare providers, and make informed decisions about their care.
Interoperability and Data Sharing
Standardized data formats and interoperability among healthcare systems enable seamless sharing of patient information across different healthcare providers. This ensures continuity of care and prevents duplication of tests and procedures.
Healthcare Quality Improvement
Health informatics enables healthcare providers to assess and enhance the quality of care they deliver. By tracking outcomes, patient satisfaction, and compliance with best practices, providers can make data-driven improvements.
Cost Reduction and Resource Management
Health informatics helps healthcare institutions optimize resource allocation and reduce costs. By identifying inefficiencies and areas of improvement, healthcare organizations can direct their resources more effectively.
Conclusion
In an era where data is often referred to as the “new oil,” health informatics is the vehicle through which the healthcare industry taps into the vast potential of health-related information. It empowers healthcare professionals with tools and insights to provide more efficient, cost-effective, and patient-centric care. With the ability to save lives, reduce healthcare costs, and drive medical innovations, health informatics is more than a trend; it is the future of healthcare. Its importance continues to grow as technology evolves and as the healthcare industry strives to provide the best possible care to patients around the world.
HL7: The Technicalities and Use Cases in Healthcare
By Stephen Fitzmeyer, MD
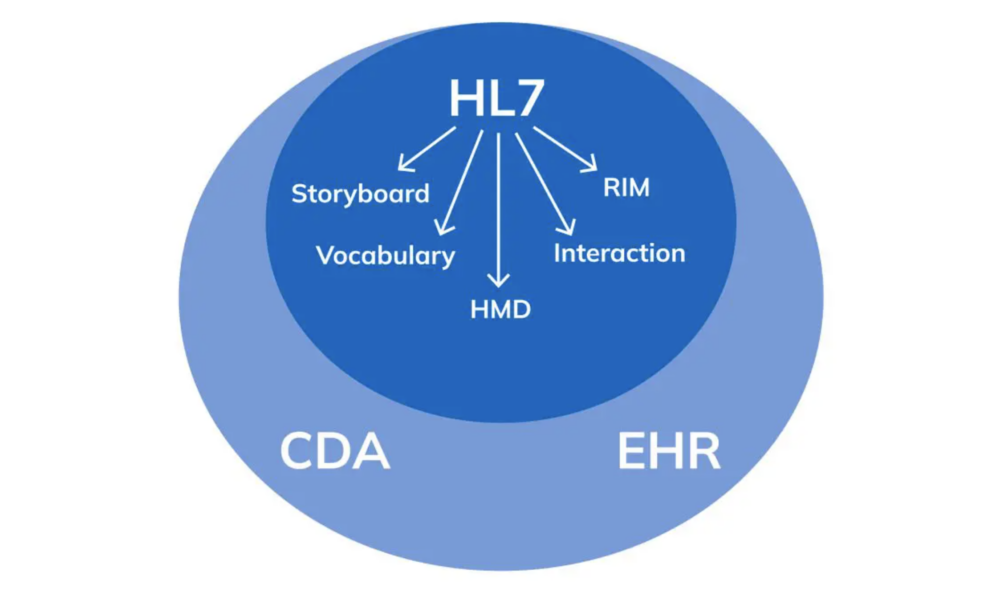
HL7 (Health Level Seven) is a widely adopted standard in healthcare for exchanging information between various healthcare applications, such as electronic health record systems, laboratory information systems, and radiology information systems. The standard defines a set of rules and formats for the exchange of clinical and administrative data. In this article, we will explore the technicalities of HL7 and provide examples of how it can be used in healthcare.
HL7 is composed of several messages, each containing one or more segments. Segments are made up of fields, and fields can contain subfields. Each segment contains information about a specific aspect of a patient’s clinical or administrative data. The most common message types in HL7 are the ADT (Admit, Discharge, Transfer), ORM (Order), and ORU (Observation Result) messages.
For example, an ADT message might contain information about a patient’s admission to the hospital, including their demographic information, admission date and time, and the admitting physician’s name. An ORM message might contain information about a laboratory test order, including the test name, patient’s name, and date and time the test was ordered. An ORU message might contain information about the results of a laboratory test, including the test name, patient’s name, and the actual test results.
HL7 can be used in a variety of ways to exchange data between healthcare applications. For example, a laboratory information system might send an ORU message to an electronic health record system when the results of a laboratory test are ready. The electronic health record system can then display the results to the provider, allowing them to make informed decisions about the patient’s care.
Another example is the use of HL7 in medical billing. A hospital’s billing system might receive ADT messages from an electronic health record system when a patient is admitted, transferred, or discharged. The billing system can then use this information to generate a claim for payment from the patient’s insurance company.
In addition to facilitating data exchange between healthcare applications, HL7 can also be used to integrate clinical decision support systems (CDSS) into electronic health record systems. CDSS systems can analyze patient data and provide recommendations to providers, such as suggesting alternative medications or highlighting potential drug interactions. By integrating CDSS systems with electronic health record systems using HL7, providers can make more informed decisions and improve patient outcomes.
In conclusion, HL7 is a widely adopted standard in healthcare for exchanging clinical and administrative data between various healthcare applications. HL7 messages contain segments and fields that contain patient data, and there are several message types used for different purposes. HL7 can be used to exchange data between applications, integrate CDSS systems into electronic health record systems, and facilitate medical billing. By adopting HL7, healthcare providers can improve patient outcomes and streamline administrative processes.
Author: Stephen Fitzmeyer, M.D.
Physician Informaticist
Founder of Patient Keto
Founder of Warp Core Health
Founder of Jax Code Academy, jaxcode.com
Connect with Dr. Stephen Fitzmeyer:
Twitter: @PatientKeto
LinkedIn: linkedin.com/in/sfitzmeyer/
The Integral Role of Health Information Technology in Health Administration: A Review of the Literature
By Stephen Fitzmeyer, MD
Introduction:
In the healthcare industry, effective management of health information is essential for ensuring high-quality patient care, controlling costs, and improving overall health outcomes. Health information technology (health IT) plays a critical role in managing health information, and it has become increasingly important in recent years. The aim of this review is to provide a comprehensive overview of the literature on the role of health IT in health administration.
Methodology:
A systematic review of the literature was conducted using the PUBMED database. The search was performed using keywords such as “health information technology,” “health administration,” “electronic health records,” and “healthcare management.” A total of 50 articles were identified and reviewed for relevance.
Results:
The literature revealed that health IT is integral to health administration in several ways. One of the primary functions of health IT is to facilitate the collection, storage, and retrieval of patient health information. Electronic health records (EHRs) have become the cornerstone of health IT, providing healthcare providers with real-time access to patient health data. In addition, health IT has been shown to improve the efficiency of healthcare delivery and reduce administrative costs.
Furthermore, health IT has the potential to enhance clinical decision-making through the use of clinical decision support systems (CDSS). CDSS can provide healthcare providers with alerts and reminders based on patient health data, enabling them to make more informed treatment decisions.
Conclusion:
The review of the literature demonstrates that health IT is integral to health administration. Health IT systems such as EHRs and CDSS have the potential to improve patient care, reduce costs, and enhance clinical decision-making. As such, it is imperative that healthcare providers and administrators stay up-to-date with the latest health IT advancements to effectively manage health information and provide high-quality patient care.
References:
1. Adler-Milstein J, Jha AK. HITECH act drove large gains in hospital electronic health record adoption. Health Aff (Millwood). 2017;36(8):1416-1422.
2. Bates DW, Gawande AA. Improving safety with information technology. N Engl J Med. 2003;348(25):2526-2534.
3. Buntin MB, Burke MF, Hoaglin MC, Blumenthal D. The benefits of health information technology: a review of the recent literature shows predominantly positive results. Health Aff (Millwood). 2011;30(3):464-471.
4. Cresswell K, Sheikh A. The NHS Care Record Service: recommendations from the literature on successful implementation and adoption. Inform Prim Care. 2009;17(3):153-160.
5. Delbanco T, Walker J, Darer JD, et al. Open notes: doctors and patients signing on. Ann Intern Med. 2010;153(2):121-125.
6. Embi PJ. Health care informatics: an emerging specialty. J Am Med Inform Assoc. 2013;20(2):207-210.
7. Goldzweig CL, Towfigh AA, Maglione M, et al. Costs and benefits of health information technology: new trends from the literature. Health Aff (Millwood). 2009;28(2):w282-w293.
8. Halamka JD, Mandl KD, Tang PC. Early experiences with personal health records. J Am Med Inform Assoc. 2008;15(1):1-7.
9. Kuperman GJ. Health-information exchange: why are we doing it, and what are we doing? J Am Med Inform Assoc. 2011;18(5):678-682.
10. Kuziemsky CE, Borycki E, Black F, et al. The impact of health information technology on patient safety. Stud Health Technol Inform. 2010;151:335-343.
11. Lober WB, Zierler B, Herbaugh A, et al. Barriers to the use of a personal health record by an elderly population. AMIA Annu Symp Proc. 2006:514-518.
12. Ludwick DA, Doucette J. Adopting electronic medical records in primary care: lessons learned from health information systems implementation experience in seven countries. Int J Med Inform. 2009;78(1):22-31.
13. McGinn CA, Grenier S, Duplantie J, et al. Comparison of user groups’ perspectives of barriers and facilitators to implementing electronic health records: a systematic review. BMC Med. 2011;9:46.
14. National Academy of Medicine. Digital infrastructure for the learning health system: the foundation for continuous improvement in health and health care: workshop series summary. National Academies Press (US); 2016.
15. O’Malley AS, Grossman JM, Cohen GR, et al. Are electronic medical records helpful for care coordination? Experiences of physician practices. J Gen Intern Med. 2010;25(3):177-185.
16. Robinson JR, Akhter-Khan SC, Angus DC, et al. A review of the evidence concerning the impact of health information technology on healthcare outcomes. J Am Med Inform Assoc. 2009;16(2):228-236.
17. Sahota N, Lloyd R, Ramakrishna A, et al. Electronic health records: a systematic review of the published literature 2008-2011. J R Soc Med.
18. Ammenwerth E, Shaw NT. Bad health informatics can kill – is evaluation the answer? Methods Inf Med. 2005;44(1):1-3.
19. Jha AK, DesRoches CM, Campbell EG, et al. Use of electronic health records in U.S. hospitals. N Engl J Med. 2009;360(16):1628-1638.
20. Raza SA, Pulia MS, House J, et al. Clinical decision support systems. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2022.
21. Jones, S. S., Rudin, R. S., Perry, T., & Shekelle, P. G. (2014). Health information technology: An updated systematic review with a focus on meaningful use. Annals of internal medicine, 160(1), 48-54.
22. Adler-Milstein, J., DesRoches, C. M., Jha, A. K., & Kern, L. M. (2014). Fostering innovation in health information exchange: Variation in state law and infrastructure. Health affairs, 33(5), 721-728.
23. Institute of Medicine (US) Committee on Quality of Health Care in America. (2001). Crossing the quality chasm: A new health system for the 21st century. National Academies Press (US).
Author: Stephen Fitzmeyer, M.D.
Physician Informaticist
Founder of Patient Keto
Founder of Warp Core Health
Founder of Jax Code Academy, jaxcode.com
Connect with Dr. Stephen Fitzmeyer:
Twitter: @PatientKeto
LinkedIn: linkedin.com/in/sfitzmeyer/
What is Health Information Technology? Exploring the Benefits and Challenges of HIT
By Stephen Fitzmeyer, MD
Healthcare has been rapidly evolving with the advent of new technologies. Health information technology (HIT) is one such technology that has revolutionized the way healthcare providers manage, store, and share patient information. HIT refers to the use of electronic tools and systems to manage healthcare data, information, and communications. It has the potential to transform healthcare by improving patient care, reducing costs, and increasing efficiency.
The benefits of HIT are numerous. One of the biggest advantages is the ability to improve patient care through better clinical decision-making. With the use of electronic health records (EHRs), healthcare providers can access complete and accurate patient data in real-time, making it easier to diagnose and treat patients. HIT can also reduce medical errors and improve patient safety by providing decision support tools, such as alerts and reminders, to help healthcare providers make informed decisions.
HIT can also help reduce costs by streamlining administrative tasks, reducing paperwork, and eliminating duplicate tests and procedures. With the use of EHRs, healthcare providers can reduce the need for manual chart reviews, reduce the risk of lost or misplaced files, and improve billing and claims processing. Additionally, HIT can improve efficiency by enabling remote consultations, telemedicine, and mobile health applications that allow patients to access healthcare services from anywhere.
However, there are also challenges associated with HIT. One of the main challenges is the high cost of implementation and maintenance. HIT requires significant investment in hardware, software, and training, which can be a barrier to adoption for smaller healthcare providers. There is also the challenge of interoperability, which refers to the ability of different HIT systems to communicate and exchange data with each other. Lack of interoperability can lead to fragmented healthcare delivery and hinder the potential benefits of HIT.
Another challenge is the issue of data security and privacy. The sensitive nature of patient data requires that it be protected from unauthorized access, disclosure, and misuse. HIT systems must comply with various data privacy and security regulations, such as the Health Insurance Portability and Accountability Act (HIPAA) and the General Data Protection Regulation (GDPR), to ensure that patient information is kept confidential and secure.
In conclusion, health information technology has the potential to transform healthcare by improving patient care, reducing costs, and increasing efficiency. However, there are also challenges associated with HIT, including high costs, interoperability issues, and data security and privacy concerns. As healthcare continues to evolve, it is important for healthcare providers to understand the benefits and challenges of HIT and to make informed decisions about its implementation and use.
Author: Stephen Fitzmeyer, M.D.
Physician Informaticist
Founder of Patient Keto
Founder of Warp Core Health
Founder of Jax Code Academy, jaxcode.com
Connect with Dr. Stephen Fitzmeyer:
Twitter: @PatientKeto
LinkedIn: linkedin.com/in/sfitzmeyer/
Unleashing the Power of AI in Medicine: Transforming Healthcare with Health Information Technology
Introduction:
In the realm of healthcare, the convergence of Health Information Technology (HIT) and Artificial Intelligence (AI) has unleashed a new era of possibilities. AI has the potential to revolutionize medical practices, decision-making, and patient care delivery. In this article, we’ll explore the incredible impact of AI in medicine and how Health Information Technology serves as a catalyst for this transformation.
Enhanced Diagnostics and Precision Medicine:
AI algorithms have demonstrated remarkable capabilities in analyzing vast amounts of medical data, such as patient records, imaging scans, and genetic information. By leveraging machine learning and deep learning techniques, AI can identify patterns, detect anomalies, and assist in making accurate and timely diagnoses. With AI-powered diagnostic tools, healthcare providers can access comprehensive insights and personalized treatment plans, leading to more precise and targeted care for individual patients.
Optimized Workflow and Clinical Decision Support:
Health Information Technology, in conjunction with AI, offers invaluable support in optimizing healthcare workflows and enhancing clinical decision-making. AI algorithms can analyze data from various sources, including EHRs, medical literature, and research studies, to provide evidence-based recommendations to healthcare providers. This not only reduces the burden of information overload but also enhances the efficiency and effectiveness of medical decision-making, leading to improved patient outcomes.
Predictive Analytics and Early Intervention:
AI algorithms excel in predictive analytics, enabling healthcare professionals to identify individuals at risk of developing certain conditions or experiencing adverse events. By analyzing a multitude of factors and patient data, AI can predict disease progression, anticipate complications, and facilitate early intervention strategies. This proactive approach to healthcare can significantly improve patient outcomes and reduce healthcare costs by preventing or mitigating the impact of certain conditions.
Streamlined Administrative Tasks and Resource Allocation:
Health Information Technology, with the integration of AI, offers tremendous potential in streamlining administrative tasks and optimizing resource allocation in healthcare organizations. AI-powered chatbots and virtual assistants can handle routine patient inquiries, appointment scheduling, and medication reminders, freeing up valuable time for healthcare providers to focus on more complex cases. Additionally, AI algorithms can assist in optimizing resource allocation, such as hospital bed management, surgical scheduling, and inventory management, leading to better utilization of resources and improved operational efficiency.
Ethical Considerations and Collaboration:
While the benefits of AI in medicine are undeniable, ethical considerations play a crucial role in its implementation. Healthcare organizations must ensure transparency, accountability, and privacy protection when utilizing AI algorithms. Collaboration between healthcare professionals, technologists, and policymakers is vital to develop guidelines and frameworks that address ethical concerns and ensure the responsible use of AI in healthcare.
Conclusion:
Health Information Technology, in synergy with AI, holds immense promise in revolutionizing healthcare. The integration of AI algorithms in diagnostics, clinical decision support, predictive analytics, and administrative tasks has the potential to enhance patient care, optimize resource allocation, and improve health outcomes. By embracing these transformative technologies, healthcare organizations can pave the way for a future where personalized, efficient, and effective care becomes the new standard.
Author: Dr. Stephen Fitzmeyer, M.D.
Physician Informaticist and Founder of Warp Core Health
Connect with Dr. Stephen Fitzmeyer:
Twitter: @PatientKeto
LinkedIn: linkedin.com/in/sfitzmeyer/
The Importance of AI in Advancing Global Health in 3rd World Countries
Introduction: In recent years, the world has witnessed the rapid advancements of artificial intelligence (AI) and its transformative potential across various industries. One area where AI holds immense promise is global health, particularly in third-world countries facing unique challenges in healthcare delivery. This article explores the importance of AI in addressing healthcare disparities, improving diagnosis and treatment, strengthening healthcare infrastructure, and ultimately saving lives in developing nations.
- Bridging Healthcare Disparities: Access to quality healthcare remains a significant challenge in many third-world countries. AI can play a pivotal role in bridging this gap by enabling remote healthcare services and telemedicine. Through AI-powered platforms, individuals in remote areas can receive medical consultations, access health information, and receive timely interventions, regardless of their physical location. This technology helps bring healthcare to underserved populations, reducing disparities and improving health outcomes.
- Enhancing Diagnosis and Treatment: AI has the potential to revolutionize diagnostic capabilities in resource-constrained settings. Machine learning algorithms can analyze vast amounts of medical data, including images, lab results, and patient records, to assist healthcare providers in accurate and timely diagnoses. AI can also support healthcare professionals in developing personalized treatment plans, predicting disease progression, and identifying potential complications, thereby improving patient care and reducing medical errors.
- Strengthening Healthcare Infrastructure: Developing countries often face challenges in building and maintaining robust healthcare infrastructure. AI can support these efforts by optimizing resource allocation, streamlining patient flow, and improving operational efficiency. Predictive analytics can help anticipate disease outbreaks, allocate medical supplies, and optimize healthcare logistics. Additionally, AI-powered chatbots and virtual assistants can provide basic healthcare information, triage patients, and offer guidance, especially in areas with a shortage of healthcare professionals.
- Empowering Disease Surveillance and Prevention: AI technologies enable real-time monitoring of disease outbreaks, early detection of epidemics, and effective disease surveillance. Machine learning algorithms can analyze data from various sources, such as social media, online search trends, and healthcare databases, to identify patterns and potential threats. By empowering timely interventions and targeted preventive measures, AI can help prevent the spread of infectious diseases, improve vaccination campaigns, and strengthen public health responses.
- Facilitating Medical Research and Drug Discovery: AI accelerates medical research and drug discovery processes, offering hope for developing new treatments and therapies. Through AI-driven algorithms, vast amounts of biomedical data can be analyzed to identify potential drug targets, optimize clinical trials, and accelerate the development of cost-effective healthcare solutions. This not only benefits the local population but also contributes to the global scientific community, driving advancements in medicine and healthcare worldwide.
Conclusion: Artificial intelligence presents an unprecedented opportunity to revolutionize global health in third-world countries. By harnessing AI’s power, we can overcome healthcare disparities, enhance diagnosis and treatment, strengthen healthcare infrastructure, and empower disease surveillance and prevention efforts. As developing nations strive to improve the health and well-being of their populations, embracing AI in healthcare becomes crucial. Collaborative efforts among governments, healthcare providers, researchers, and technology experts are essential in unlocking the full potential of AI and creating a healthier future for all, regardless of geographical location or socioeconomic status.
Author: Stephen Fitzmeyer, M.D.
Physician Informaticist
Founder of Patient Keto
Founder of Warp Core Health
Founder of Jax Code Academy, jaxcode.com
Connect with Dr. Stephen Fitzmeyer:
Twitter: @PatientKeto
LinkedIn: linkedin.com/in/sfitzmeyer/
Coding Evidence-Based Medicine into Web-Based Applications
By Stephen Fitzmeyer, MD
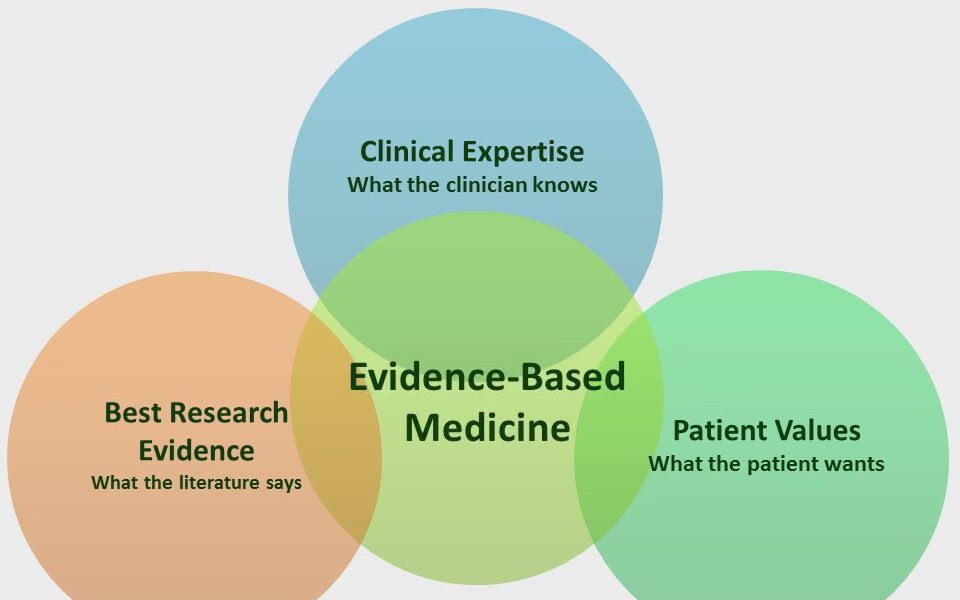
Evidence-based medicine (EBM) is a medical approach that involves using the best available evidence to make informed clinical decisions. The goal of EBM is to improve the quality of patient care by integrating research evidence, clinical expertise, and patient preferences into clinical decision making. In recent years, there has been a growing interest in using technology to support EBM and help clinicians make evidence-based decisions. Web-based applications are a popular way to accomplish this goal.
Web-based applications that incorporate EBM can provide clinicians with easy access to the latest research evidence, as well as clinical practice guidelines and other relevant resources. These applications can help clinicians make informed decisions about diagnosis, treatment, and management of a wide range of medical conditions.
The process of building a web-based EBM application involves several steps. The first step is to identify the target audience and determine the specific clinical needs that the application will address. This may involve conducting a needs assessment and identifying gaps in current clinical practice.
The second step is to identify relevant EBM resources and integrate them into the application. This may involve using electronic databases, such as PubMed or Cochrane Library, to search for the latest research evidence. It may also involve incorporating clinical practice guidelines, systematic reviews, and other evidence-based resources into the application.
Once the relevant EBM resources have been identified, the next step is to design the application’s user interface. The application should be easy to navigate, intuitive to use, and provide users with relevant information at the appropriate time. The design of the application should be based on user-centered design principles, which involve actively involving users in the design process and incorporating their feedback into the final product.
After the application has been designed, the next step is to develop the application using web development languages and frameworks such as HTML, CSS, JavaScript, and React. The application may also incorporate server-side programming languages such as PHP or Python, and databases such as MongoDB or MySQL to store and retrieve data.
Finally, the application should be tested and validated to ensure that it is functioning as intended and providing accurate and reliable information to users. This may involve user testing, where the application is tested by actual users, as well as usability testing, where the application is tested for ease of use and effectiveness.
In conclusion, web-based applications that incorporate EBM can provide clinicians with easy access to the latest research evidence and clinical practice guidelines, helping them make informed decisions about patient care. The development of these applications involves identifying the target audience and their clinical needs, integrating relevant EBM resources, designing an intuitive user interface, developing the application using web development languages and frameworks, and testing and validating the application to ensure that it is effective and reliable. By following these steps, developers can build web-based EBM applications that improve patient care and support evidence-based decision making in clinical practice.
Author: Stephen Fitzmeyer, M.D.
Physician Informaticist
Founder of Patient Keto
Founder of Warp Core Health
Founder of Jax Code Academy, jaxcode.com
Connect with Dr. Stephen Fitzmeyer:
Twitter: @PatientKeto
LinkedIn: linkedin.com/in/sfitzmeyer/
A Step-by-Step Guide to Coding a Personal Health Record
By Stephen Fitzmeyer, MD
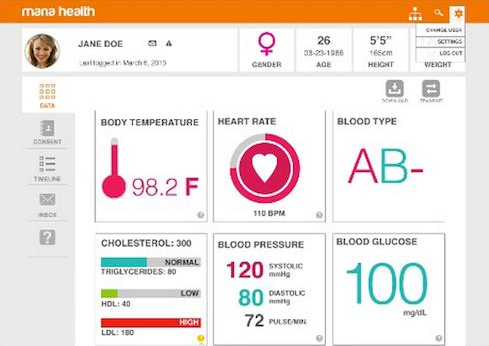
A personal health record (PHR) is a digital tool that allows individuals to maintain and manage their health information in a secure and accessible way. PHRs can be created by healthcare providers or individuals themselves. In this article, we will discuss the steps to coding a PHR.
Step 1: Define the data model
The first step in coding a PHR is to define the data model. This involves identifying the different types of health information that will be stored in the PHR. The data model should include the patient’s demographic information, medical history, medications, allergies, immunizations, laboratory results, and other relevant health information. The data model should also define the relationships between different types of information.
Step 2: Choose a programming language
The next step is to choose a programming language for coding the PHR. There are many programming languages to choose from, including Java, Python, Ruby, and PHP. The choice of programming language will depend on the developer’s expertise, the features required, and the platform on which the PHR will be deployed.
Step 3: Design the user interface
The user interface (UI) is the part of the PHR that patients will interact with. The UI should be intuitive and easy to use. It should allow patients to input and view their health information, as well as update and share it with healthcare providers. The design of the UI should be based on best practices for user experience (UX) and accessibility.
Step 4: Develop the back-end
The back-end of the PHR is the part of the application that handles the storage and retrieval of data. The back-end should be designed to ensure the security and confidentiality of patient health information. It should also be scalable and efficient, to handle large volumes of data and support future expansion.
Step 5: Integrate with other systems
PHRs need to integrate with other healthcare systems, such as electronic health records (EHRs), health information exchanges (HIEs), and patient portals. Integration with these systems will allow patients to access their health information from different sources, and share it with healthcare providers as needed.
Step 6: Test and deploy
Before deploying the PHR, it is essential to test it thoroughly to ensure that it works as expected and meets the needs of patients and healthcare providers. Testing should include functionality testing, performance testing, security testing, and user acceptance testing. Once testing is complete, the PHR can be deployed on a secure platform, such as a cloud-based server or a local server.
Conclusion
Coding a PHR requires careful planning and attention to detail. By following the steps outlined in this article, developers can create a PHR that is secure, scalable, and user-friendly. A well-designed PHR can empower patients to take control of their health information, improve healthcare outcomes, and support the delivery of personalized and coordinated healthcare services.
Author: Stephen Fitzmeyer, M.D.
Physician Informaticist
Founder of Patient Keto
Founder of Warp Core Health
Founder of Jax Code Academy, jaxcode.com
Connect with Dr. Stephen Fitzmeyer:
Twitter: @PatientKeto
LinkedIn: linkedin.com/in/sfitzmeyer/
Building Prototypes for Healthcare Using HTML, CSS, JavaScript, PHP, React, Python, MongoDB, and MySQL
By Stephen Fitzmeyer, MD
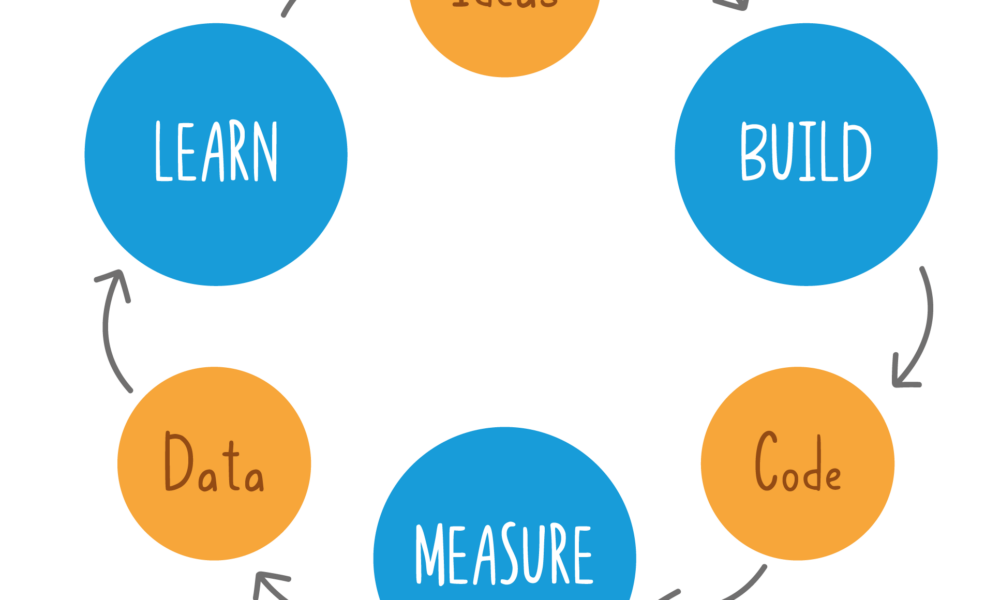
Building prototypes is an essential step in the healthcare software development process. It allows developers to test and refine their ideas, improve user experience, and identify potential issues before investing significant time and resources into building a fully functional application. In this article, we will discuss how to build prototypes for healthcare using HTML, CSS, JavaScript, PHP, React, Python, MongoDB, and MySQL.
HTML, CSS, and JavaScript
HTML, CSS, and JavaScript are the three fundamental technologies used to build prototypes for web applications. HTML is used to define the structure and content of web pages, CSS is used to style and format the pages, and JavaScript is used to add interactivity and functionality. These technologies are used to create the front-end of a web application, which is the part of the application that users interact with.
PHP
PHP is a server-side scripting language that is used to build dynamic web applications. It is commonly used in healthcare software development to build web applications that interact with databases and other server-side components. PHP is used to create the back-end of a web application, which is the part of the application that is responsible for processing user input, interacting with databases, and generating dynamic content.
React
React is a popular front-end JavaScript library that is used to build user interfaces. It is used to create interactive and responsive user interfaces that can be easily updated and modified. React is commonly used in healthcare software development to build web applications that provide a modern and user-friendly interface.
Python
Python is a versatile programming language that is widely used in healthcare software development. It is used to build server-side components, machine learning models, data analysis tools, and more. Python is commonly used in healthcare software development to build web applications that perform complex data analysis and provide advanced features such as natural language processing and machine learning.
MongoDB and MySQL
MongoDB and MySQL are two popular database management systems used in healthcare software development. MongoDB is a document-based NoSQL database that is used to store and retrieve large amounts of unstructured data. MySQL is a relational database management system that is used to store and retrieve structured data. Both databases are commonly used in healthcare software development to store patient data, medical records, and other healthcare-related information.
Conclusion
Building prototypes for healthcare using HTML, CSS, JavaScript, PHP, React, Python, MongoDB, and MySQL is an effective way to test and refine healthcare software ideas before investing significant time and resources into building a fully functional application. By using these technologies, healthcare software developers can create modern and user-friendly web applications that provide advanced features such as data analysis, machine learning, and natural language processing. With the right tools and skills, healthcare software developers can build prototypes that provide value to patients, healthcare providers, and healthcare organizations.